ISSN: 0970-938X (Print) | 0976-1683 (Electronic)
Biomedical Research
An International Journal of Medical Sciences
Research Article - Biomedical Research (2017) Volume 28, Issue 18
Ultrasound guided high intensity focused ultrasound for advanced pancreatic cancer: A comparative study between Chinese and Bulgarian patients
Kun Zhou1*, Dobromir Dimitrov Dimitrov2, Hyuliya Erdzhanova Feradova2, Wei Yang1, Lifeng Ran1, Grigor Angelov Gorchev2, Chengbing Jin1, Slavcho Tomov2, Hui Zhu1, Tashko Deliyski2, Zhibiao Wang3 and Zhechuan Mei1
1Clinical Center for Tumor Therapy, the Second Affiliated Hospital of Chongqing Medical University, Chongqing, PR China
2Medical University Pleven, Pleven, Bulgaria
3College of Biomedical Engineering, Chongqing Medical University, Chongqing, PR China
- *Corresponding Author:
- Kun Zhou
Clinical Center for Tumor Therapy
The Second Affiliated Hospital of Chongqing Medical University, PR China
Accepted date: August 24, 2017
Objective: This study is to determine the efficacy of the Chinese clinical program of Ultrasound Guided High-Intensity Focused Ultrasound (USgHIFU) in the Bulgarian patients with advanced pancreatic adenocarcinoma.
Methods: Patients with advanced pancreatic adenocarcinoma from China and Bulgaria were enrolled in the study. All patients received the same clinical procedure of USgHIFU treatment and follow-up. The patient characteristics, the USgHIFU treatment and evaluation parameters including complications, Visual Analogue Scale (VAS) pain scores, tumor size, serum CA19-9 levels, survival rates and survival times were comparatively studied in Chinese and Bulgarian patients.
Results: There was no significant difference in clinical parameters of Chinese and Bulgarian patients with advanced pancreatic adenocarcinoma, such as the ratio of male/female, mean age, tumor size, and TNM stage. Similarly, no statistical significance was found in USgHIFU procedure including treatment time, the ratio of USgHIFU time to treatment time, USgHIFU time, average power and total energy. After USgHIFU treatment, four patients with complications were recorded. The VAS pain scores post- USgHIFU were decreased. Besides, the tumor shrunk after treatment, and the one-year survival rate for the Chinese and Bulgarian patients were 26.0% and 37.0%, respectively. The results showed no statistical significance between patients from China and Bulgaria. Additionally, the serum CA19-9 content did not show significant change in Chinese and Bulgarian patients after USgHIFU treatment.
Conclusion: A good consistency in treatment efficacy of USgHIFU was found in Chinese and Bulgarian patients with advanced pancreatic adenocarcinoma, suggesting that the Asian-originated USgHIFU treatment for advanced pancreatic adenocarcinoma may be also suitable for European patients.
Keywords
Ultrasound guided high-intensity focused ultrasound (USgHIFU), Advanced pancreatic cancer, Cancerrelated pain, Survival rate
Introduction
Pancreatic cancer is one of the malignancies that are most difficult to diagnose and with worst outcomes. The 5 y survival rate of pancreatic cancer is less than 5% [1-3]. It is reported that the mortality of pancreatic cancer ranks the fourth of all malignancies in Europe and North America [1-3]. In China, pancreatic cancer is the top 10 [4,5] cause of cancer related death and is the fifth in Bulgaria [2,6].
So far, R0 resection (complete surgical removal of tumor) is still the only curative method for early pancreatic cancer. Unfortunately, most of patients with pancreatic cancer are difficult to diagnose at the initial period due to the non-specific early symptoms. Only 20% of pancreatic cancer patients in early stage are suitable for surgical resection, and expected to have a 5 y survival rate of 15%-20% [7-10]. The majority of patients (80%) with advanced pancreatic cancer (including local and tumor metastasis) is expected to have a median survival time less than one year and 5 y survival rate nearly 0% due to lack of the alternative effective treatment [7-10].
High-Intensity Focused Ultrasound (HIFU) has been used for treatment of solid tumors (regardless of benign and malignant) in Asia and Europe [11-13]. Studies have shown that the Ultrasound guided HIFU (USgHIFU) method achieved better therapeutic effects on Asian patients with advanced pancreatic cancer [14-24]; however, its application in European patients has not been well investigated [25]. In addition to pancreatic adenocarcinoma [26,27], USgHIFU is also suitable for the treatment of pancreatic neuroendocrine tumor [28,29], pancreatic cystadenocarcinoma [30], acinic cell carcinoma [30], and pancreatic metastatic cancer [28]. According to the clinical guideline of USgHIFU treatment [31], we designed this study and investigated whether this USgHIFU treatment also benefits Bulgarian patients with advanced pancreatic adenocarcinoma.
Materials and Methods
Clinical teams for USgHIFU treatment
This study was separately performed in the Second Affiliated Hospital of Chongqing Medical University (Chongqing, China) and the Affiliated Hospital of Medical University Pleven (Pleven, Bulgaria) at the same time. Clinical team in the Second Affiliated Hospital of Chongqing Medical University has more than 15 years of experience in USgHIFU treatment, however, the clinical team in Medical University Pleven only has 2 years of experience. Besides, doctors in both of the two teams have more than 10 years of clinical experience of diagnosis and treatment of pancreatic cancer.
Patients
This study was approved by the Ethics Committee of the Second Affiliated Hospital of Chongqing Medical University and the Medical University Pleven. The informed consents were obtained from patients and their family before procedures. The inclusion criteria included: i) patients with pathologically diagnosed pancreatic adenocarcinoma; ii) TNM stage III/IV; iii) Karnofsky score above 70%; iv) expected survival time more than three months. The exclusion criteria included: i) patients with un-controlled cardio-pulmonary diseases, ii) patients with active hemorrhagic diseases, including upper gastric-intestinal bleeding, iii) patients with Child-Pugh Grade C liver disease; iv) patients with continuous and increasing jaundice, and v) patients with large scar in the acoustic pathway of HIFU on the abdominal wall. From January 2013 to January 2015, 49 advanced pancreatic adenocarcinoma patients (including local and tumor metastasis) without surgical options were enrolled in this study. These 49 patients included 27 Chinese patients and 22 Bulgarian patients. Their clinical characteristics were shown in Table 1. There was no significant difference in clinical characteristics between Chinese patients and Bulgarian patients.
| Clinical characteristics | Chinese patients | Bulgarian patients | Statistical data |
|---|---|---|---|
| Number of cases | 27 | 22 | |
| Sex M/F | 20/7 | 14/8 | χ2=0.622, P=0.430* |
| Age (years old) | |||
| Mean ± SD (range) | 58.6 ± 9.82 (35-72) | 56.7 ± 7.12(40-68) | t=0.760, P=0.451# |
| Tumor location | |||
| Head/Body/Tail | χ2=0.449, P=0.799* | ||
| Invade two parts | 8 | 4 | |
| Tumor size (mm) | |||
| Mean ± SD (range) | 40.6 ± 13.37 (20-70) | 40.0 ± 9.67 (23-62) | t=0.185, P=0.854# |
| TNM stage (III/IV) | 8/19 | 10/12 | χ2=1.306, P=0.253* |
| HIFU session (single/multiple) | 22/5 | 20/2 | χ2=0.880, P=0.348* |
| Chemotherapy (Y/N) | 6/21 | 12/10 | χ2=5.450, P=0.020* |
Table 1. The clinical characteristics of patients with advanced pancreatic cancer in two groups.
Measurement of biochemical indicators
The routine examination, including Electrocardiograph, chest X-ray, enhanced Computed Tomography (CT)/Magnetic Resonance Imaging (MRI), blood cell counting, and serum CA19-9 level, was performed before USgHIFU treatment. The pain score was evaluated by Visual Analogue Scale (VAS) [32].
USgHIFU equipment
The JC USgHIFU system (Chongqing Haifu Medical Technology Co. Ltd., Chongqing, China) was applied on Chinese and Bulgarian patients. The therapeutic procedure was guided by a real-time B-mode ultrasound. A DU3 US imaging device with 2.5-3.5 MHz imaging probe (Esaote, Genova, Italy) was used as the real-time imaging unit of the system. Therapeutic ultrasound energy was produced by a transducer with diameter about 150 mm diameter, focal length about 135 mm, and work frequency about 0.85 MHz.
USgHIFU treatment
Bowel preparation was performed one day before USgHIFU, and a routine fasting and water-deprivation should be finished 10 h before USgHIFU. Patients lay down on the table of JC USgHIFU system after anesthesia. A tank containing degassed water was used to fulfil the space between the body and the transducer in order to create an acoustic pathway without air bubbles. Besides, in order to get rid of gas left in the bowels (potentially in the acoustic pathway), a water balloon was placed between the abdominal wall and the transducer.
The basic mode of HIFU treatment was shown as dot-lineslice- volume. Guided by real-time monitoring B modeultrasound, targeted lesion was accurately located, and further divided into slices. Normally, it began from one dot, gradually became a line, then a slice, and eventually a volume. The USgHIFU treatment was finished if the hyper-echogenic changes fulfilled the whole targeted lesion. The USgHIFU treatment targeted tumors not only located in pancreas but also in distance metastases.
The parameters of USgHIFU including treatment time, USgHIFU time, average power and total energy were separately recorded. The treatment time was the time duration started from the first therapeutic ultrasound exposure to the last one. The USgHIFU time was the sum of all therapeutic ultrasound exposure time. The average power and total energy were recorded and calculated by JC USgHIFU system.
Follow-up study
Vital signs of patients were closely monitored for at least 6 hours after USgHIFU treatment. All patients were encouraged to do activity and suggested no meal before passing air again. The clinical assessment was performed after USgHIFU operation, and the complication was recorded one week post- USgHIFU by referring to CTCAE3.0 grade [33]. The pain score was evaluated by VAS pre-and post-USgHIFU. The concentration of amylase and CA19-9 in serum of patients was also tested. One month after USgHIFU, radiography (enhanced CT/MRI) was performed to measure the lesion size. Additionally, a follow-up was performed every three months to study the survival condition of patients. The follow-up lasted for 24 months from January 2013 to January 2015.
Chemotherapy
The adjuvant gemcitabine-based chemotherapy, which included 4-6 cycles, was recommended to patients. Patients who finished chemotherapy were recorded as “Yes Chemotherapy”, and those who refused or did not finished were recorded as “No Chemotherapy”.
Statistical analysis
Data was analysed using SPSS version 19.0 for Windows (SPSS Inc., Chicago, US). Continuous variables were shown as Mean ± SD, and analysed by independence t-test. The level of serum CA19-9 and VAS pain score before and after USgHIFU treatment were comparatively analysed by paired t-test. Statistical analysis of categorical values was performed by Chisquare test. The duration of a patient’s survival was calculated from the date of USgHIFU treatment to the date of death. The cumulative survival rate was estimated by Kaplan-Meier method and compared by Log-Rank test. It was considered as statistical significance if P<0.05.
Results
Comparison of USgHIFU parameters between Chinese and Bulgarian patients
To evaluate the differences of the USgHIFU procedure between the two groups, multiple comparisons of USgHIFU parameters were performed. There was no significant difference in USgHIFU treatment between Chinese and Bulgarian patients by analysis of the USgHIFU parameters, including treatment time, HIFU time, average power and total energy, as shown in Table 2.
| Parameters of USgHIFU | Chinese patients | Bulgarian patients | Statistical data |
|---|---|---|---|
| Number of cases | 27 | 22 | |
| USgHIFU session | 32 | 24 | |
| Treatment time (min) | |||
| Mean ± SD (range) | 119.6 ± 72.08 (8-254) | 156.6 ± 57.32 (20-285) | t=-1.955, P=0.057* |
| HIFU time (min) | |||
| Mean ± SD (range) | 22.8 ± 9.4 (2.35-37.38) | 17.9 ± 11.57 (4.5-55) | t=1.644, P=0.107* |
| Average power (W) | |||
| Mean ± SD (range) | 281.8 ± 46.5 (200-407) | 270.0 ± 94.43 (95-400) | t=0.569, P=0.572* |
| Total energy (kJ) | |||
| Mean ± SD (range) | 392.0 ± 188.46 (41.5-672.9) | 303.2 ± 217.29 (28-881) | t=1.531, P=0.132* |
Table 2. The parameters of USgHIFU treatment for patients with advanced pancreatic cancer in two groups.
Comparison of VAS pain score between Chinese and Bulgarian patients
To evaluate the changes of the VAS pain score after USgHIFU treatment, VAS pain score was collected before and one-week post-USgHIFU treatment. The result showed that the VAS pain score of patients with advanced pancreatic adenocarcinoma significantly decreased in Chinese patients and Bulgarian patients after USgHIFU treatment (Table 3, P<0.001). Besides, in Chinese patients, 14 patients felt pain relief (51.9%), 10 patients felt no change (37.4%) and 3 patients (11.1%) felt pain increase; while these three conditions in Bulgarian patients were 14 (63.6%), 6 (27.3%) and 1 (4.5%). There was no significant difference in the constituent ratios of the three conditions (pain relief/no change/increase) between the Chinese and Bulgarian patients after USgHIFU treatment (Table 3). These results indicate that a similar pain control is achieved in Chinese and Bulgarian patients after USgHIFU treatment.
| Total number | VAS scores | Number of patients with VAS scores modification | ||||||
|---|---|---|---|---|---|---|---|---|
| pre-USgHIFU | post-USgHIFU | Statistical data* | Decrease | No change | Increase | Statistical data# | ||
| Chinese patients | 27 | 5.3 ± 3.14 | 3.1 ± 2.01 | t=3.876, P= 0.001 | 14 | 10 | 3 | χ2=1.270 |
| Bulgarian patients | 21 | 5.8 ± 3.01 | 2.9 ± 1.92 | t =4.254, P<0.001 | 14 | 6 | 1 | P=0.530 |
Table 3. Evaluation of the VAS pain scores for patients with advanced pancreatic cancer in two groups before and after HIFU treatment.
Comparison of complications and outcome between Chinese and Bulgarian patients
To evaluate the complications after USg HIFU treatment, follow-up was conducted. During follow-up, four patients with complications were reported one-month post-USgHIFU (Table 4). Two patients had pancreatitis (Grade 1). There was no symptom, but only with higher level of serum amylase, which reduced to normal level in one week without any medical intervention. The other two patients suffered skin burn (Grade 2), and the burn wound healed after debridement in one week. No serious complication was found, and all patients suffering complications recovered in one week. The complication ratio in Chinese patients was 1:27 while in Bulgarian patients was 3:22. No statistical significance was found between the two groups (P>0.05).
| Complications | Patient Number/ CTCAE 3.0 Grade | Outcome | ||
|---|---|---|---|---|
| Chinese patients | Bulgarian patients | Total | ||
| Gastrointestinal Tract injury | 0 | 0 | 0 | No record. |
| Skin burn | 0 | 2/Grade 2 | 2 | Due to the previous surgery scare, debridement was performed, and the wound healed in 1 week. |
| Pancreatitis | 1/Grade 1 | 1/Grade 1 | 2 | Serum-amylase level back to normal in one week. No treatment was needed. |
| Total | 1 | 3 | 4 | |
Table 4. Number and CTCAE3.0 grade of complications and outcome.
Comparison of tumor size between Chinese and Bulgarian patients
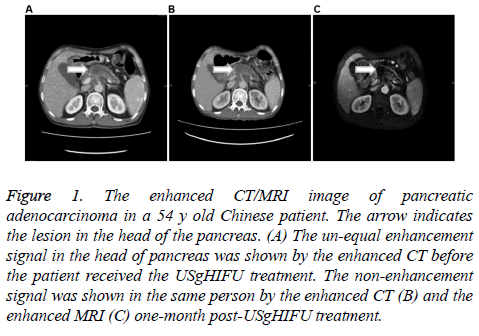
To study the tumor size change after USgHIFU treatment, the enhanced CT/MRI was performed and data was further analysed by paired t-test. The results showed that the tumor shrunk after USgHIFU treatment in both two groups. No statistical significance was found in tumor size in Chinese patients (P>0.05). However, the USgHIFU treatment significantly decreased the tumor size in Bulgarian patients (P<0.05, Table 5 and Figure 1).
Figure 1: The enhanced CT/MRI image of pancreatic adenocarcinoma in a 54 y old Chinese patient. The arrow indicates the lesion in the head of the pancreas. (A) The un-equal enhancement signal in the head of pancreas was shown by the enhanced CT before the patient received the USgHIFU treatment. The non-enhancement signal was shown in the same person by the enhanced CT (B) and the enhanced MRI (C) one-month post-USgHIFU treatment.
| Group | Pre-HIFU | Post-HIFU | Statistical analysis | |||
|---|---|---|---|---|---|---|
| N | Size (mm) (Mean ± SD) | N | Size (mm) (Mean ± SD) | Method | P value | |
| Chinese patients | 20 | 39.8 ± 12.58 | 20 | 36.8 ± 12.43 | Paired t-test | 0.032 |
| Bulgarian patients | 12 | 34.6 ± 4.25 | 12 | 29.5 ± 5.43 | 0.015 | |
Table 5. The modification of tumor size in patients with advanced pancreatic cancer after USgHIFU treatment in two groups.
Comparison of CA19-9 level between Chinese and Bulgarian patients
To assess the level of tumor marker CA19-9 in Chinese and Bulgarian patients after USgHIFU treatment, the serum of 21 Chinese patients and 5 Bulgarian patients one-month post- USgHIFU were collected. Our data showed that serum CA19-9 level of patients in Chinese patients decreased after USgHIFU treatment from 554.1 ± 379.94 to 527.9 ± 389.9 (P=0.733), while in Bulgarian patients, it also showed decline trend from 30.7 ± 23.81 to 23.0 ± 17.49 (P=0.386) (Table 6).
| Group | N | Pre-USgHIFU | Post-USgHIFU | Statistical data |
|---|---|---|---|---|
| Chinese patients* | 21 | 554.1 ± 379.94 (16.95-1000) | 527.9 ± 389.9 (5.38-1000) | t=0.347, P=0.733 |
| Bulgarian patients# | 5 | 30.7 ± 23.81 (5.5-62.28) | 23.0 ± 17.49 (1.9-39.6) | t=0.972, P=0.386 |
| The maximum limit was 1000 U/ml. That datum over 1000 U/ml was treated as 1000 U/ml. | ||||
| Paired t-test. P<0.05 means significant difference. | ||||
Table 6. Comparison of the serum CA19-9 (U/ml) level in Chinese and Bulgarian patients with advanced pancreatic cancer pre- and post- USgHIFU treatment.
Comparison of survival time between Chinese and Bulgarian patients
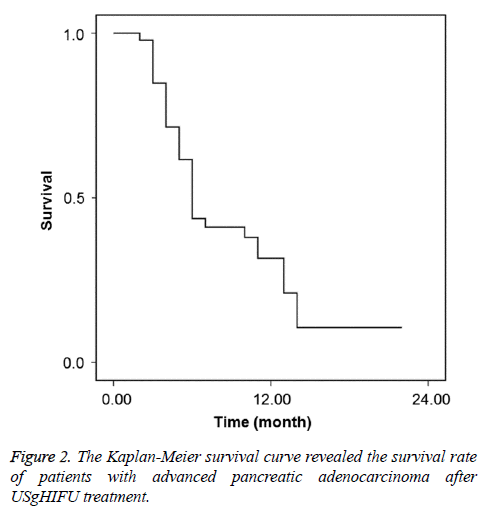
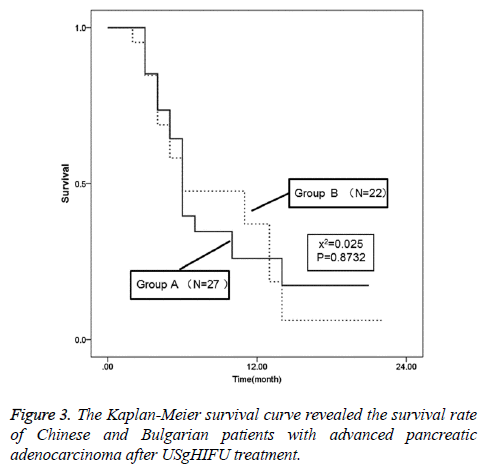
To study the long term survival condition of patients after USgHIFU treatment, the survival rate was analysed. For all patients after USgHIFU treatment, the survival rate at 6 month, 12 month and 18 month was 43.6%, 31.6% and 10.5%, respectively (Figure 2), whilst the mean survival time and the median survival time were 8.9±0.95 and 6.0 ± 0.43 months. For Chinese patients, the survival rate after USgHIFU treatment at 6 month, 12 month and 18 month was 39.6%, 26.0% and 17.3%, respectively; while that in Bulgarian patients was 47.6%, 37.0% and 6.2%, respectively. There was no significant difference in the survival rate between the two groups (P=0.873, Figure 3). Additionally, the mean/median survival time for Chinese patients and Bulgarian patients was 8.9 ± 1.45/6.0 ± 0.43 and 8.9 ± 1.26/6.0 ± 3.25 months, respectively.
Discussion
Patients from China and Bulgarian diagnosed with advancer pancreatic adenocarcinoma were involved in this study, and received the same USgHIFU treatment in Chinese and Bulgarian Hospital, respectively. The Second Affiliated Hospital of Chongqing Medical University has performed USgHIFU treatment for more than 15 y, while, the hospital of Medical University Pleven has performed USgHIFU for only 2 y. To avoid the treatment differences, we comparatively analysed the clinical characteristics of patients in two hospitals as well as their USgHIFU treatment parameters. No statistical significance was found between Chinese patients and Bulgarian patients, which indicate that the USgHIFU treatment is suitable for both Chinese and Bulgarian patients, even with different clinical teams.
Clinical studies have reported the complications of pancreatic cancer after HIFU treatment, which involved skin burn [14,16-19,21-22,24] and pancreatitis [19,23,24], superior mesenteric artery insufficiency occlusion [16], pancreaticoduodenal fistula [17,19] and obstructive jaundice [22,24]. Most of the complications need simple medical intervention. Here, we found the complications after USgHIFU treatment in this study were similar as previously reported.
Several studies have confirmed that the HIFU treatment could relieve the cancer-related pain by ablating the local pancreatic cancer and its distance metastasis including plexus celiacus and retroperitoneal nerve plexus [24,25,31-37]. The previous metaanalysis has shown that 80% of pancreatic cancer patients benefited from HIFU treatment, and among those, 30% of patients felt pain-free [38], which was important to improve the life quality. Additionally, studies have demonstrated that the serum CA19-9 levels showed no changes after HIFU treatment [14,19,23]. Consistently, we found that there was no significant difference in serum CA19-9 after HIFU treatment in both Chinese and Bulgarian patients. Besides, in agreement of the previous studies which demonstrated the tumor size shrunk after HIFU treatment [14-23], our data also supported the decrease tendency of ablated pancreatic cancer after USgHIFU treatment. Meanwhile, clinical studies [15,18,19,23] have also indicated the one-year survival rate of Asian patients with advanced pancreatic cancer after USgHIFU treatment was 14.3%-49.9% and the median survival time was 7-12 months. Our study obtained consistent results in patient survival.
So far, few European patients with pancreatic cancer have been reported to receive HIFU treatment [25]. The HIFU treatment is safe and effective in the Asian patients [11,12,14-24]. In agreement with that, our study not only confirmed the treatment effect of USgHIFU on Chinese patients with advanced pancreatic adenocarcinoma, but also revealed a similar therapeutic efficacy on Bulgarian patients. Our findings indicate that USgHIFU treatment might be an alternative choice for European patients with advanced pancreatic adenocarcinoma.
Acknowledgements
This work was supported by Graduate student research innovation project of Chongqing Municipal Education Commission (No. CYS14106) and by Frontier and application basic research of Committee of Science and Technology of Chongqing grant (No.cstc2013jcyjA0267) and by the Chongqing Science and Technology Program for Public Wellbeing (No. cstc2015jcsf10002-14).
Declaration of Conflicts of Interest
All authors declare no financial competing interests. All authors declare no non-financial competing interests.
References
- Malvezzi M, Bertuccio P, Levi F, La Vecchia C, Negri E. European cancer mortality predictions for the year 2013. Ann Oncol 2013; 24: 792-800.
- Ferlay J, Steliarova-Foucher E, Lortet-Tieulent J, Rosso S, Coebergh JW, Comber H, Forman D, Bray F. Cancer incidence and mortality patterns in Europe: Estimates for 40 countries in 2012. Eur J Cancer 2013; 49: 1374-1403.
- Siegel R, Ma J, Zou Z, Jemal A. Cancer statistics, 2014. CA Cancer J Clin 2014; 64: 9-29.
- Chen W, Zheng R, Zhang S, Zhao P, Li G. Report of incidence and mortality in China cancer registries, 2009. Chin J Cancer Res 2013; 25: 10-21.
- Chen W, Zheng R, Zhang S, Zhao P, Zeng H. Report of cancer incidence and mortality in China, 2010. Ann Transl Med 2014; 2: 61.
- Dimitrova N, Vukov M, Valerianova Z. Cancer Incidence in Bulgaria, 2009. Sofia, Bulgaria: AVIS-24 Ltd. 2011; 14-15.
- Clinical guideline for pancreatic cancer. Chinese Clin Oncol 2011; 16: 1026-1032.
- He J, Page AJ, Weiss M, Wolfgang CL, Herman JM, Pawlik TM. Management of borderline and locally advanced pancreatic cancer: Where do we stand? World J Gastroenterol 2014; 20: 2255-2266.
- Ghosn M, Kourie HR, El Karak F, Hanna C, Antoun J, Nasr D. Optimum chemotherapy in the management of metastatic pancreatic cancer. World J Gastroenterol 2014; 20: 2352-2357.
- Keane MG, Bramis K, Pereira SP, Fusai GK. Systematic review of novel ablative methods in locally advanced pancreatic cancer. World J Gastroenterol 2014; 20: 2267-2278.
- Zhang L, Wang ZB. High-intensity focused ultrasound tumor ablation: review of ten years of clinical experience. Front Med China 2010; 4: 294-302.
- Orsi F, Arnone P, Chen W, Zhang L. High intensity focused ultrasound ablation: a new therapeutic option for solid tumors. J Cancer Res Ther 2010; 6: 414-420.
- Orgera G, Monfardini L, Della Vigna P, Zhang L, Bonomo G, Arnone P, Padrenostro M, Orsi F. High-intensity focused ultrasound (HIFU) in patients with solid malignancies: evaluation of feasibility, local tumour response and clinical results. Radiol Med 2011; 116: 734-748.
- Zhu H, Chen WZ, Wu F. High intensity focused ultrasound in the treatment of pancreatic cancer. Chinese J Ultrasound Med 2003; 19: 306-308.
- Wu F, Wang ZB, Zhu H, Chen WZ, Zou JZ, Bai J, Li KQ, Jin CB, Xie FL, Su HB. Feasibility of US-guided high-intensity focused ultrasound treatment in patients with advanced pancreatic cancer: initial experience. Radiology 2005; 236: 1034-1040.
- Wang W, Tang J, Ye HY. Ablation effects of high-intensity focused ultrasound therapy on pancreatic cancer. Chinese J Ultrasound Med 2007; 23: 76-79.
- Song IH, Jung SE, Hahn ST. High-intensity focused ultrasound treatment (HIFU) for the advanced pancreatic cancer. J Korean Radiol Soc 2007; 56: 555-562.
- Wang K, Liu L M, Chen Z. High-intensity focused ultrasound therapy for advanced pancreatic carcinoma. Chinese J Ultrasound Med 2010; 26: 373-376.
- Sung HY, Jung SE, Cho SH, Zhou K, Han JY. Long-term outcome of high-intensity focused ultrasound in advanced pancreatic cancer. Pancreas 2011; 40: 1080-1086.
- Wang K, Chen L, Meng Z, Lin J, Zhou Z, Wang P, Chen Z. High intensity focused ultrasound treatment for patients with advanced pancreatic cancer: A preliminary dosimetric analysis. Int J Hyperthermia 2012; 28: 645-652.
- Yan T, Lu W, Zhang J H. The research of injury mechanism on acoustic pathway of high intensity focused ultrasound treatment for pancreatic cancer. Chinese J Inj Rep Wound Heal 2013; 8: 193-197.
- Wang K, Zhu H, Meng Z, Chen Z, Lin J. Safety evaluation of high-intensity focused ultrasound in patients with pancreatic cancer. Onkologie 2013; 36: 88-92.
- Gao HF, Wang K, Meng ZQ, Chen Z, Lin JH, Zhou ZH, Wang P, Shi WD, Sheng YH. High intensity focused ultrasound treatment for patients with local advanced pancreatic cancer. Hepatogastroenterol 2013; 60:1906-1910.
- Lu W, Wang D. Effects of HIFU on relieving the pain of advanced pancreatic cancer. J Hepatopancreatobil Surg 2014; 26: 105-108.
- Orsi F, Zhang L, Arnone P, Orgera G, Bonomo G, Vigna PD, Monfardini L, Zhou K, Chen W, Wang Z, Veronesi U. High-intensity focused ultrasound ablation: effective and safe therapy for solid tumors in difficult locations. AJR Am J Roentgenol 2010; 195: 245-252.
- Dimitrov D, Andreev T, Feradova H, Ignatov B, Zhou K. Multimodality treatment by FOLFOX plus HIFU in a case of advanced pancreatic carcinoma. A case report. JOP 2015; 16: 66-69.
- Marinova M, Rauch M, Mücke M. High-intensity focused ultrasound (HIFU) for pancreatic carcinoma: evaluation of feasibility, reduction of tumour volume and pain intensity. Eur Radiol 2016; 26: 1-10.
- Orgera G, Krokidis M, Monfardini L, Arnone P, Bonomo G, Della Vigna P, Curigliano G, Orsi F. Ultrasound-Guided High-Intensity Focused Ultrasound (USgHIFU) ablation in pancreatic metastasis from renal cell carcinoma. Cardiovasc Intervent Radiol 2012; 35: 1258-1261.
- Chen Q, Zhu X, Chen Q, Wang K, Meng Z. Unresectable giant pancreatic neuroendocrine tumor effectively treated by high-intensity focused ultrasound: A case report and review of the literature. Pancreatology 2013; 13: 634-638.
- Wang RS, Mu QX, Liu LX. A clinical study of thermotherapy of HIFU in combination with chemotherapy on treating advanced pancreatic cancer. Acta Academiae Medicinae Nanjing 2003.
- Clinical guideline for pancreatic cancer. 2009 Fudan University Shanghai Cancer Center. (http://www.shca.org.cn/UploadFiles/20091089240503.doc)
- Wewers ME, Lowe NK. A critical review of visual analogue scales in the measurement of clinical phenomena. Res Nurs Health 1990; 13: 227-236.
- Cancer Therapy Evaluation Program. Common terminology criteria for adverse events. Version 3.0, DCTD, NCI, NIH, DHHS 2003. (http://ctep.cancer.gov/protocolDevelopment/electronic_applications/docs/ctcaev3.pdf)
- Chaussy CG, Thuroff S. Transrectal high-intensity focused ultrasound for local treatment of prostate cancer: current role. Arch Esp Urol 2011; 64: 493-506.
- Huber PE, Jenne JW, Rastert R, Simiantonakis I, Sinn HP, Strittmatter HJ, von Fournier D, Wannenmacher MF, Debus J. A new noninvasive approach in breast cancer therapy using magnetic resonance imaging-guided focused ultrasound surgery. Cancer Res 2001; 61: 8441-8447.
- Ruhnke H, Eckey T, Bohlmann MK, Beldoch MP, Neumann A, Agic A, Hägele J, Diedrich K, Barkhausen J, Hunold P. MR-guided HIFU treatment of symptomatic uterine fibroids using novel feedback-regulated volumetricablation: effectiveness and clinical practice. ROFO 2013; 184: 983-991.
- Bohlmann MK, Hoellen F, Hunold P, David M. High-intensity focused ultrasound ablation of uterine fibroids-potential impact on fertility and pregnancy outcome. Geburtshilfe Frauenheilkd 2014; 74: 139-145.
- Jia L, Xie B. A meta-analysis of high intensity focused ultrasound (HIFU) therapy on pain relief in pancreatic cancer. Chinese J Pancreatol 2008; 8: 13-15.