ISSN: 0970-938X (Print) | 0976-1683 (Electronic)
Biomedical Research
An International Journal of Medical Sciences
Research Article - Biomedical Research (2017) Volume 28, Issue 13
The use of medial stabilization and the sinus tarsi approach to treat Sanders type II and III calcaneal fractures
Jian Zou, Zhongmin Shi*, Jianfeng Xue, Wenqi Gu, Guohua Me and Xiaolin Li
Department of Orthopedics, Shanghai Jiao Tong University Affiliated Sixth People’s Hospital, Shanghai 200233, PR China
- *Corresponding Author:
- Zhongmin Shi
Department of Orthopedics
Shanghai Jiao Tong University Affiliated Sixth People’s, Hospital, PR China
Accepted on May 25, 2017
The aim of this study was to assess the clinical outcomes of surgical treatment for displaced intraarticular calcaneal fractures using a mini-fragment locking plate, via the modified sinus tarsi approach. In this retrospective study, 16 patients (13 men and 3 women) with 16 displaced intra-articular calcaneal fractures were included. A modified sinus tarsi approach was used to reduce and stabilize the posterior facet. This was done using the raft technique with a mini-fragment locking plate, and multiple sagittal screws were added percutaneously, to stabilize the calcaneal body and control rotation. Intra-operative three-dimensional computed tomography was routinely performed to evaluate the reduction and screw placement. The pre- and postoperative Böhler and Gissane angles were compared. The mean duration of follow-up was 18.4 months. The mean union time was 10 weeks. The mean preoperative Böhler angle (13.4° ± 3.0°) and Gissane angle (88.1° ± 4.5°) were significantly increased (P<0.05) at the final follow-up (26.5° ± 5.4° and 116.2° ± 7.7°, respectively). The mean postoperative AOFAS and SF-36 scores were 83.3 and 79.5, respectively. Complications included two cases of moderate subtalar joint stiffness. No wound edge necrosis, superficial or deep infection, or nerve injury was observed in these patients. The application of minimally invasive raft technique using a mini-fragment locking plate combined with percutaneous screw fixation is an effective option for treating displaced Sanders type II and III intraarticular calcaneal fractures.
Keywords
Intra-articular calcaneal fractures, Displaced, Internal fixation, Minimally invasive, Percutaneous.
Introduction
The most suitable treatment for displaced intra-articular calcaneal fractures is still controversial. Since the mid-1990s, open reduction and internal fixation (ORIF) via the extensile lateral approach [1-3] has been considered the standard treatment for displaced intra-articular fractures of the calcaneus, as it generally restores the subtalar joint anatomically and has good functional outcomes. However, there are multiple complications of open surgery including peroneal tendonitis (18%), sural nerve injury (9%), flap devascularization with surgical wound dehiscence (6-33%), infection (8-18%), and amputation (0-2%) [4-6]. Owing to the high risk of soft-tissue complications associated with the more invasive lateral approach and plating, a minimally invasive treatment with limited internal fixation was proposed to decrease the risk of these complications. Many different limited open approaches (e.g., the Palmer approach, Smileincision, Ollier approach, and sinus tarsi approach) and fixation techniques (e.g., K-wires, screws, 1/3-tube plate, and staples) were reported to be effective for treating intra-articular calcaneal fractures in small-scale studies [7-9]. Unfortunately, there is no consensus on the optimum minimally invasive treatment technique for displaced intra-articular calcaneal fractures. Herein, we describe our experience of using a novel surgical approach for displaced intra-articular calcaneal fracture repair, consisting of a limited sinus tarsi approach, and mini-fragment locking plate raft technique [10,11].
The objectives of this study were to present a surgical technique of medial stabilization and ORIF for displaced intraarticular calcaneal fractures using a raft technique with a minifragment locking-plate to evaluate the clinical and radiological outcomes after a minimum follow-up of 1 year and to compare the results obtained with previous data reported in literature.
Subjects and Methods
Subjects
Between February 2010 and February 2011, 16 displaced intraarticular calcaneal fractures in 16 patients were managed surgically by performing limited open reduction via a sinus tarsi approach using locking plate internal fixation. All patients were surgically treated at a single level one-trauma center by the same surgeon (Shi ZM). The indication for surgical treatment was a more than 2 mm displacement of the posterior facet of the subtalar joint, with a decrease in the Böhler angle and widening of the heel.
Among the 16 patients included in this study, 13 were men and 3 women. The average age was 40.6 years (range, 24-56 years) and average BMI was 22.8 kg/m2. Fourteen patients were involved in labor work, one worked in an office and one was a homemaker. The right side was involved in 10 patients and the left side in 6 patients. The injury was sustained because of a fall from a height in 12 patients and a motor vehicle accident in 4 patients. All cases were closed fractures. Five young adult patients were smokers (but not heavy smokers) and were instructed to stop smoking until complete wound healing. Only one patient had diabetes, but the condition was controlled. Two patients had associated injuries (Table 1).
| No. | Sex | fracture type | Age (yrs) | Follow-up time (m) | Operation duration (min) | Union time (w) | AOFAS | SF-36 | VAS | Böhler angle pre-operation (°) | Böhler angle postoperation (°) | Böhler angle at last follow-up (°) | Gissane angle pre-operation (°) | Gissane angle postoperation (°) | Gissane angle at last follow-up (°) |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1 | M | IIA | 28 | 22 | 75 | 16 | 78 | 90 | 0 | 10 | 33 | 31 | 87 | 100 | 96 |
| 2 | M | IIIAB | 39 | 20 | 80 | 12 | 76 | 77 | 1 | 17 | 20 | 18 | 94 | 117 | 113 |
| 3 | M | IIIBC | 41 | 17 | 80 | 10 | 89 | 85 | 1 | 11 | 22 | 22 | 92 | 123 | 123 |
| 4 | F | IIA | 43 | 17 | 80 | 12 | 86 | 90 | 1 | 8 | 21 | 19 | 79 | 111 | 107 |
| 5 | M | IIA | 38 | 12 | 90 | 12 | 78 | 76 | 0 | 10 | 38 | 38 | 83 | 116 | 116 |
| 6 | M | IIIAC | 24 | 19 | 85 | 9 | 89 | 85 | 1 | 11 | 23 | 21 | 86 | 103 | 103 |
| 7 | F | IIB | 41 | 14 | 75 | 12 | 85 | 82 | 1 | 13 | 26 | 26 | 87 | 118 | 118 |
| 8 | M | IIA | 44 | 18 | 80 | 12 | 77 | 84 | 1 | 16 | 22 | 22 | 89 | 120 | 118 |
| 9 | M | IIC | 38 | 16 | 70 | 20 | 86 | 73 | 2 | 12 | 25 | 25 | 95 | 124 | 124 |
| 10 | F | IIA | 56 | 19 | 60 | 12 | 91 | 72 | 2 | 19 | 21 | 21 | 81 | 122 | 122 |
| 11 | M | IIA | 49 | 24 | 70 | 12 | 79 | 88 | 1 | 14 | 26 | 24 | 92 | 119 | 119 |
| 12 | M | IIIAB | 52 | 21 | 70 | 12 | 58 | 60 | 7 | 14 | 35 | 33 | 86 | 118 | 114 |
| 13 | M | IIA | 34 | 22 | 90 | 11 | 87 | 72 | 0 | 11 | 32 | 30 | 94 | 123 | 123 |
| 14 | M | IIIAB | 45 | 18 | 80 | 16 | 89 | 73 | 1 | 17 | 24 | 22 | 88 | 102 | 102 |
| 15 | M | IIB | 39 | 17 | 85 | 16 | 95 | 92 | 1 | 15 | 25 | 25 | 89 | 121 | 117 |
| 16 | M | IIB | 39 | 18 | 85 | 14 | 90 | 73 | 1 | 16 | 31 | 31 | 88 | 122 | 118 |
| mean | 40.6 | 18.4 | 78.4 | 13.0 | 83.3 | 79.5 | 1.3 | 13.4 | 26.5 | 25.5 | 88.1 | 116.2 | 114.6 | ||
| std | 7.8 | 3.0 | 7.8 | 2.7 | 8.6 | 8.6 | 1.6 | 3.0 | 5.4 | 5.6 | 4.5 | 7.7 | 8.4 |
Table 1. The basic information of patients.
Initially, patients were treated using the “R.I.C.E” (Rest, Ice, Compression, Elevation) principle. Splinting materials were not used, and active muscular contraction of the injured foot was encouraged to decrease the swelling. Imaging studies included axial and lateral radiography of the calcaneus and anteroposterior and oblique radiography of the injured foot. Computed tomography (CT) was also routinely performed. Fractures were classified according to the Sanders classification system [12]. Lateral and axial radiography scans were evaluated to calculate the Böhler angle and the length, height, and width of the calcaneus. Comparisons were made between the injured and non-injured foot.
There were 11 cases of Sanders type II fractures: 7 type IIA, 3 type IIB, and 1 type IIC. Five cases comprised type III fractures: 3 type IIIAB, 1 type IIIAC, and 1 type IIIBC. Surgery was performed after an average duration of 4.83 days from admission (range, 1-11 days). The study was approved by the Shanghai Sixth People’s Hospital. All patients provided written informed consent for their participation in the trial and for all additional measurements.
Surgical technique
Surgery was performed after the swelling had subsided. Patients were placed in a prone position, and the affected limb was exsanguinated before applying a tourniquet. The ankle was elevated using medical dressing to facilitate eversion of the subtalar joint during reduction and fixation of the posterior facet.
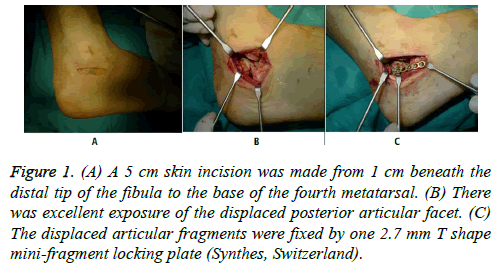
A 5 cm skin incision was made from 1 cm beneath the distal tip of the fibula to the base of the fourth metatarsal bone (Figure 1A). The superficial dermis, deep dermis, and subcutaneous tissue were carefully incised in layers. The peroneal tendon was inferiorly identified, and the fat overlying the sinus tarsi in the proximal aspect of the incision and the fascia centrally overlying the extensor digitorum brevis were removed. The peroneal tendons were retracted plantarly to expose the anterior aspect of the posterior calcaneal facet. The extensor digitorum brevis tendons were stripped dorsally to expose the calcaneocuboid joint.
Figure 1: (A) A 5 cm skin incision was made from 1 cm beneath the distal tip of the fibula to the base of the fourth metatarsal. (B) There was excellent exposure of the displaced posterior articular facet. (C) The displaced articular fragments were fixed by one 2.7 mm T shape mini-fragment locking plate (Synthes, Switzerland).
The lateral wall of the calcaneus was then exposed via sharp dissection with a thin periosteal elevator and retracted like a door to expose the depressed fracture fragment. After sharp dissection of any remaining capsular tissue and washing out the fracture hematoma, it was possible to inspect the displaced posterior articular facet (Figure 1B). One 4.0 mm K-wire was inserted into the calcaneal turberosity from the lateral side, and traction was applied toward the bottom to correct the calcaneal varus deformity. The fracture at the medial wall was then reduced by inserting a narrow Langenbeck elevator deep into the medial wall along the original fracture line. After correcting the varus deformity, height, and length, one 2.0 mm K-wire was inserted to fix the medial column temporarily along the medial wall to the sustentaculum tali. Axial radiographs of the calcaneus were obtained to check the reduction of the medial wall, alignment of the tuberosity, and direction of the medial K-wire. The posterior facet was reduced using the K-wire and Langenbeck elevator and fixed to the sustentaculum tali temporarily using one or two 1.5-mm Kwires. While the lateral wall was impacted by compressing the heel to reduce the calcaneal width, another 2.0-mm K-wire was inserted into the anterior process to stabilize the tuberosity with the anterior portion and to support the posterior facet. If the anterior fracture line extended to the calcaneocuboid joint, transverse lag screws were used to fix fractures of the anterior process.
A 2.7 mm T-shaped mini-fragment locking plate with six to seven holes (Synthes, Switzerland) was selected for all the procedures. After being pre-bended according to the shape of the lateral wall, the locking plate was placed immediately beneath the posterior facet (Figure 1C). The locking plate could not only support the posterior facet by the “raft technique”, but could also connect the posterior portion to the anterior process. The use of the raft technique indicates that 3-4 parallel screws were placed into the subchondral bone to support the articular surface. The last step was the percutaneous positioning of cannulated screws through the posterior tuberosity directed toward the calcaneocuboid joint. The screw length was 65-70 mm at all times, which allowed us to maintain reduction of the extra-articular component and to support the articular component.
Before closure of the wound, 3D-CT scanning (Siemens, Germany) was performed to check the screw position and posterior facet reduction. Finally, the soft-tissue flap was reduced, and the operative wound closed in two layers using a suction drain.
Postoperative management
A night splint was used until the foot was partially weightbearing. The “R.I.C.E” (Rest, Ice, Compression, Elevation) principle was also applied postoperatively to decrease the swelling. As soon as the patient was comfortable and the wound healed (7-10 days postoperatively), exercises for subtalar motion were encouraged, including assisted active circumduction, inversion, and eversion movements of the heel in order to re-establish motion of the subtalar joint. Sutures were removed 3 weeks after surgery, following which gentle strengthening exercises were performed for the muscles controlling the foot and ankle. The foot was allowed to be partially weight bearing with walking boots and crutches until the fracture had healed, as observed on radiography, which was usually by 8-10 weeks. Thereafter, full weight bearing without support was gradually resumed over a period of 4-6 weeks.
Follow-up
Patients were evaluated clinically and radiologically after 1, 3, 6, and 12 months. Follow-up included axial and lateral radiographs, CT-scans, and measurement of the Böhler and Gissane angles (in lateral view) of the operated and the contralateral calcaneus. The criteria of bone union were the absence of pain or tenderness at the fracture site while bearing weight and bridging of the fracture site on radiographs. The angles were measured manually on physical radiographs with a goniometer. Furthermore, follow-up included assessment of a range of motions (pro-/supination and dorsal extension/plantar flexion) of the affected and contralateral side, pain according to a visual analogue scale (VAS) (0=no pain, 10=maximum imaginable pain), the American Orthopaedic Foot and Ankle Society (AOFAS) Ankle-Hindfoot score, and the short-form (SF-36) health survey. All radiographs were reviewed by an experienced radiologist and by another foot and ankle surgeon for signs of osteoarthritis and bony consolidation. The final clinical and radiological assessment was performed by an independent observer who had not been involved in the operative treatment. Loss of reduction was defined as the appearance of a ≥ 2 mm displacement of the joint or body of the calcaneus, or a change of ≥ 5° in the Böhler angle on any of the follow-up radiographs.
Statistical evaluation
The data were compiled and analyzed using the commercial software program, SPSS version 13.0 (SPSS, Chicago, IL). Continuous data obeyed normal distribution, and they were expressed as mean values ± standard deviation. Comparisons between different time points were made using paired Student t-tests. A significant result was taken as P<0.05.
Results
No patients were lost to follow-up. Normal alignment of the calcaneus, including heel height and width, and adequate restoration of the joint surface with incongruity of less than 2 mm, were obtained in all patients of this study, as judged clinically and radiographically. Two patients experienced subtalar joint stiffness without traumatic arthritis, but no patient required a secondary subtalar fusion. No case of wound edge necrosis, incision infection, hematoma, or nerve injury was observed in this study. On radiography, there was no screw loosening, implant break, nonunion, or malunion.
All patients had a stable plantigrade foot without signs of axial deviation or chronic swelling. Eight patients (80%) did not experience any pain during their daily activities and work, while two reported occasional pain while walking on uneven terrain or down stairs. All patients wore normal footwear, and no orthopedic devices were required.
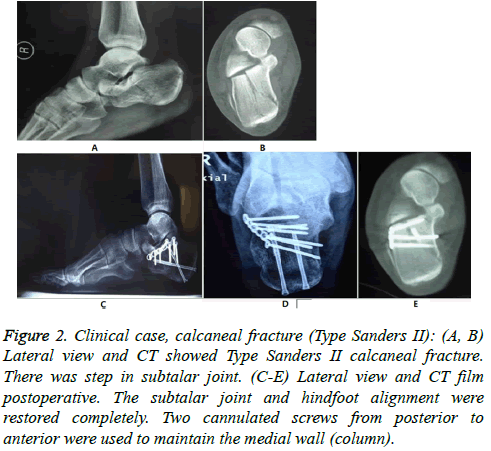
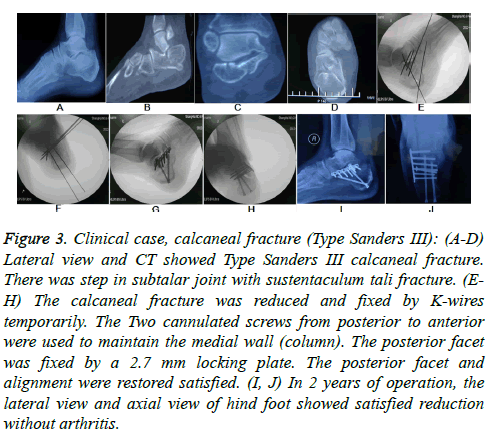
Both Böhler and Gissane angles were increased postoperatively (t=8.234, P<0.001; t=12.26, P<0.001). Though both angles were decreased at last follow-up, the values were not significantly different from those at post-operation (t=0.506, P=0.616; t=0.565, P = 0.576) (Figures 2 and 3 and Table 1).
Figure 2: Clinical case, calcaneal fracture (Type Sanders II): (A, B) Lateral view and CT showed Type Sanders II calcaneal fracture. There was step in subtalar joint. (C-E) Lateral view and CT film postoperative. The subtalar joint and hindfoot alignment were restored completely. Two cannulated screws from posterior to anterior were used to maintain the medial wall (column).
Figure 3: Clinical case, calcaneal fracture (Type Sanders III): (A-D) Lateral view and CT showed Type Sanders III calcaneal fracture. There was step in subtalar joint with sustentaculum tali fracture. (EH) The calcaneal fracture was reduced and fixed by K-wires temporarily. The Two cannulated screws from posterior to anterior were used to maintain the medial wall (column). The posterior facet was fixed by a 2.7 mm locking plate. The posterior facet and alignment were restored satisfied. (I, J) In 2 years of operation, the lateral view and axial view of hind foot showed satisfied reduction without arthritis.
Discussion
Although the extended lateral approach has been used widely to treat calcaneal fractures, it is associated with a high rate of soft-tissue complications, including dehiscence of the wound, deep infection, peroneal tendonitis, tarsal tunnel syndrome, and compartmental syndrome, which may occur in 6-30% of patients [4,13,14]. Recently, many modified minimally invasive techniques have been proposed, including the Ilizarov device [15], percutaneously applied distraction systems [16,17], and percutaneous arthroscopy-assisted osteosynthesis [18,19], all of which result in improved prognosis but have a long learning curve. However, in literature, calcaneocuboid reduction has been rarely mentioned or assessed. It is very difficult to reduce and maintain the anterior facet via a percutaneous technique. However, via the sinus tarsi approach, the anterior and posterior facets can be easily exposed, visualized, and simultaneously reduced and fixed using one small plate.
Palmer [20] originally described a lateral approach through the sinus tarsi for direct visualization of the articular surface for reduction. However, it may be necessary to extend the limits of a small incision over the sinus tarsi to treat adjacent fractures or to aid reduction in case of more complex fractures. We have used an extended sinus tarsi approach to allow percutaneous placement of a plate beneath the lateral calcaneal skin flap through a sinus tarsi approach and to treat adjacent fractures and soft tissue injuries.
In 2000, Ebraheim et al. [21] described a sinus tarsi approach with minimal internal fixation and immobilization of the subtalar joint. However, the reported infection rate (8.5%) and soft-tissue complications (9.2%) such as peroneal tendinitis, sinus tarsi syndrome, and compartment syndrome associated with this approach were even higher than those associated with the extended lateral approach. However, in a review, Schepers [22] reported that wound complications ranged from 0-15.4% (mean, 4.8%), which was much lower than the rate for the extended lateral approach. In this study, there was no case of wound edge necrosis, incision infection, or hematoma. The rate of complications was lower than that reported in previous studies [23-27]. As the sinus tarsi approach does not need to strip too much from the lateral wall, the damage to the local blood supply of the flap is less, which decreases the postoperative complications such as wound dehiscence and deep infection. It is further believed that reduction via the sinus tarsi approach could minimize the amount of scar formation and prevent stiffness of the subtalar joint. In our study, only two patients complained of subtalar joint stiffness but without functional limitation. This result was better than that previously reported in literature.
Several fixation devices using the sinus tarsi approach have been proposed. Different plates such as the circle plate, Hplate, 3.5 mm reconstruction plate, 1/3-tube plate, and Y-plate can be used to fix fractures. In our experience, the minifragment locking plate is a better choice in the sinus tarsi approach. The plate can be easily placed in the window that this approach offers, without much exposure. A locking plate can not only provide angular stability to fragments, but also maintain the height of the posterior facet, as well as prevent later subsidence. A long locking plate can also be used if the fracture involves the anterior process and turberosity. Brunner et al. [28] reported using a 2.0 mm locking plate to treat calcaneal fractures. The rate of broken implants was 16%. The 3.5 mm plate was too large, such that only two holes and screws could be used to maintain the posterior facet. In this study, a 2.7 mm locking plate was used. The length of the locking plate ranged from 40-65 mm. At least four holes and screws could be used as a “raft technique” to firmly hold the posterior facet, and no significant subsidence was seen at the last follow-up.
Intra-articular fractures require anatomic reduction and stable fixation to improve the chances of a good outcome [29-31]. The main problem associated with percutaneous fixation is a secondary loss of reduction of 3-20° in the Böhler angle [18,32]. In our study, we achieved a good correction of the Böhler angle (mean correction, 13.1° ± 3.8°) because our surgical technique provided the most stable support with triangle-shaped stability. Recently, many authors have proposed that the main goal of treatment for displaced fractures of the calcaneus should be the restoration of the threedimensional structure, with emphasis on correct alignment in the coronal and axial planes and the height of the calcaneal body, rather than anatomical reconstruction of the congruency of the subtalar articular fragments [33,34].
Although medial wall fixation is not a new concept in the treatment of calcaneal fracture, medial stabilization is first proposed by us. Maxwell et al. [35] compared the biomechanical performance between a single and dual locking plate system for an intra-articular calcaneal fracture model and demonstrated that the dual plating technique experienced a small amount of fragment translation during cycling that was significantly different from that with lateral plating. James et al. [36] suggested stabilizing the tuber by placing 2 or 3 screws longitudinally from the tuber. These screws should be placed close to the medial wall to prevent recurrence of translation and varus deformity. Ibrahim et al. [37] reported a minimum follow-up of 15 years after ORIF of calcaneus fractures, and suggested that even after years, healed calcaneal fractures may not reach the same stability as unfractured calcanei, which may lead to chronic sintering of the posterior facet because of microfractures and stress risers in the cancellous bone. Dynamic hip screw (DHS) cannot be used in intertrochanteric fracture if there is comminuted fracture in the lesser trochanter. The calcaneal fixation follows the same pattern. Plate fixation is an eccentric fixation. If there is a comminuted fracture in the medial wall, the lateral plate may not stabilize the medial side. It will cause implant failure and varus deformity. Therefore, medial stabilization using two long screws is important to maintain calcaneal length and prevent varus deformity. The calcaneus is a cancellous bone with low nonunion rate. Therefore, nonunion or delayed union cases are rarely encountered clinically, irrespective of age.
In our experience, the first step in the treatment of calcaneal fractures is to restore and maintain the alignment in the axial planes (varus deformity) with 1-2 long screws. The posterior facet can then be reduced and maintained using a 2.7 mm locking plate. We preferred the 2.7 mm locking plate with 6-7 holes. A 2.7 mm locking plate with 3-4 locking screws raft beneath the posterior facet can provide angular stability. Finally, one screw from the posterior lateral tuberosity to the anterior process can then maintain the calcaneus length. This pattern represents the three-point pattern required to maintain the arch structure. Loss of reduction did not occur in any of our patients. Although there was some late subsidence with ensuing gradual loss of the Böhler angle correction over the follow-up period, the value at the last follow-up (25.5° ± 5.6°) was not significantly different from the immediate postoperative value (26.5° ± 4.5°; t=0.56, P=0.58). One or more 2.0 mm bioabsorbable pins can be used to reinforce the stability of the posterior facet if there are some small fragments that cannot be fixed using the locking plate.
Our study has several limitations. The first limitation is the small cohort size. To determine whether this minimal invasive technique can provide a better outcome compared with the classical extensile lateral plating, evaluation of more patients, including the elderly, smokers, and diabetics, will be necessary. The second limitation is the classification of the enrolled patients. The fracture types in this study were Sanders type II and simple type III. More severe fracture patterns (Sanders type III and IV) treated using this minimal invasive technique should be tested in future studies. Thirdly, we did not have a control group of patients who underwent nonoperative or standard ORIF for comparison. Another limitation is the short follow-up period.
In conclusion, medial stabilization and the sinus tarsi approach is a satisfactory method to treat Sanders type II and III calcaneal fractures.
References
- Yao H, Liang T, Xu Y, Hou G, Lv L, Zhang J. Sinus tarsi approach versus extensile lateral approach for displaced intra-articular calcaneal fracture: a meta-analysis of current evidence base. J Orthop Surg Res 2017; 12: 43.
- Meena S, Gangary SK, Sharma P. Review Article: Operative versus nonoperative treatment for displaced intraarticular calcaneal fracture: a meta-analysis of randomised controlled trials. J Orthop Surg (Hong Kong) 2016; 24: 411-416.
- Li B, Wu G, Yang Y. Conservative versus surgical treatment for displaced fracture of the medial process of the calcaneal tuberosity. J Orthop Surg (Hong Kong) 2016; 24: 163-166.
- Kiewiet NJ, Sangeorzan BJ. Calcaneal Fracture Management: Extensile Lateral Approach Versus Small Incision Technique. Foot Ankle Clin 2017; 22: 77-91.
- Chen CH, Hung C, Hsu YC, Chen CS, Chiang CC. Biomechanical evaluation of reconstruction plates with locking, nonlocking, and hybrid screws configurations in calcaneal fracture: a finite element model study. Med Biol Eng Comput 2017.
- Wakatsuki T, Imade S, Uchio Y. Avulsion fracture of the calcaneal tuberosity treated using a side-locking loop suture (SLLS) technique through bone tunnels. J Orthop Sci 2016; 21: 690-693.
- Li LH, Guo YZ, Wang H, Sang QH, Zhang JZ, Liu Z, Sun TS. Less wound complications of a sinus tarsi approach compared to an extended lateral approach for the treatment of displaced intraarticular calcaneal fracture: A randomized clinical trial in 64 patients. Medicine (Baltimore) 2016; 95: e4628.
- Labronici PJ, Reder VR, de Araujo Marins Filho GF, Pires RE, Fernandes HJ, Mercadante MT. Risk of injury to vascular-nerve bundle after calcaneal fracture: comparison among three techniques. Rev Bras Ortop 2016; 51: 208-213.
- He XY, Wang CQ, Zhou ZP. Clinical efficacy of cannulated screw fixation with percutaneous Poking reduction for the treatment of calcaneal fracture. Zhongguo Gu Shang 2016; 29: 421-423.
- Hu SJ, Chang SM, Zhang YQ, Ma Z, Du SC, Zhang K. The anterolateral supra-fibular-head approach for plating posterolateral tibial plateau fractures: A novel surgical technique. Injury 2016; 47: 502-507.
- Wang PC, Ren D, Zhou B. Surgical Technique of Anterolateral Approach for Tibial Plateau Fracture. Orthop Surg 2015; 7: 368-370.
- Koval KJ, Sanders R. The radiologic evaluation of calcaneal fractures. Clin Orthop Relat Res 1993; : 41-46.
- Levin LS, Nunley JA. The management of soft-tissue problems associated with calcaneal fractures. Clin Orthop Relat Res 1993; 290: 151-156.
- Lim EV, Leung JP. Complications of intraarticular calcaneal fractures. Clin Orthop Relat Res 2001; : 7-16.
- Emara KM, Allam MF. Management of calcaneal fracture using the Ilizarov technique. Clin Orthop Relat Res 2005; 439: 215-220.
- Schepers T, Schipper IB, Vogels LM, Ginai AZ, Mulder PG, Heetveld MJ, Patka P. Percutaneous treatment of displaced intra-articular calcaneal fractures. J Orthop Sci 2007; 12: 22-27.
- Rammelt S, Amlang M, Barthel S, Gavlik JM, Zwipp H. Percutaneous treatment of less severe intraarticular calcaneal fractures. Clin Orthop Relat Res 2010; 468: 983-990.
- Gavlik JM, Rammelt S, Zwipp H. Percutaneous, arthroscopically-assisted osteosynthesis of calcaneus fractures. Arch Orthop Trauma Surg 2002; 122: 424-428.
- Rammelt S, Gavlik JM, Barthel S, Zwipp H. The value of subtalar arthroscopy in the management of intra-articular calcaneus fractures. Foot Ankle Int 2002; 23: 906-916.
- Palmer I. The mechanism and treatment of fractures of the calcaneus; open reduction with the use of cancellous grafts. J Bone Joint Surg Am 1948; 30A: 2-8.
- Ebraheim NA, Elgafy H, Sabry FF, Freih M, Abou-Chakra IS. Sinus tarsi approach with trans-articular fixation for displaced intra-articular fractures of the calcaneus. Foot Ankle Int 2000; 21: 105-113.
- Schepers T. The sinus tarsi approach in displaced intra-articular calcaneal fractures: a systematic review. Int Orthop 2011; 35: 697-703.
- Shuler FD, Conti SF, Gruen GS, Abidi NA. Wound-healing risk factors after open reduction and internal fixation of calcaneal fractures: does correction of Bohler's angle alter outcomes? Orthop Clin North Am 2001; 32: 187-192.
- Khorbi A, Chebil M, Ben Maitigue M, Khemiri C, Haddad N, Kanoun ML, Ben Dali N, Hachem A. Screw fixation without bone graft of calcaneal joint fractures: 35 cases. Rev Chir Orthop Reparatrice Appar Mot 2006; 92: 45-51.
- Xia S, Lu Y, Wang H, Wu Z, Wang Z. Open reduction and internal fixation with conventional plate via L-shaped lateral approach versus internal fixation with percutaneous plate via a sinus tarsi approach for calcaneal fractures - a randomized controlled trial. Int J Surg 2014; 12: 475-480.
- Zhang T, Su Y, Chen W, Zhang Q, Wu Z, Zhang Y. Displaced intra-articular calcaneal fractures treated in a minimally invasive fashion: longitudinal approach versus sinus tarsi approach. J Bone Joint Surg Am 2014; 96: 302-309.
- Rawicki N, Wyatt R, Kusnezov N, Kanlic E, Abdelgawad A. High incidence of post-operative infection after 'sinus tarsi' approach for treatment of intra-articular fractures of the calcaneus: a 5 year experience in an academic level one trauma center. Patient Saf Surg 2015; 9: 25.
- Brunner A, Muller J, Regazzoni P, Babst R. Open reduction and internal fixation of OTA type C2-C4 fractures of the calcaneus with a triple-plate technique. J Foot Ankle Surg 2012; 51: 299-307.
- Abdelazeem A, Khedr A, Abousayed M, Seifeldin A, Khaled S. Management of displaced intra-articular calcaneal fractures using the limited open sinus tarsi approach and fixation by screws only technique. Int Orthop 2014; 38: 601-606.
- Buckley R, Leighton R, Sanders D, Poon J, Coles CP, Stephen D, Paolucci EO. Open reduction and internal fixation compared with ORIF and primary subtalar arthrodesis for treatment of Sanders type IV calcaneal fractures: a randomized multicenter trial. J Orthop Trauma 2014; 28: 577-583.
- Hsu AR, Anderson RB, Cohen BE. Advances in Surgical Management of Intra-articular Calcaneus Fractures. J Am Acad Orthop Surg 2015; 23: 399-407.
- Stulik J, Stehlik J, Rysavy M, Wozniak A. Minimally-invasive treatment of intra-articular fractures of the calcaneum. J Bone Joint Surg Br 2006; 88: 1634-1641.
- Kikuchi C, Charlton TP, Thordarson DB. Limited sinus tarsi approach for intra-articular calcaneus fractures. Foot Ankle Int 2013; 34: 1689-1694.
- Yeo JH, Cho HJ, Lee KB. Comparison of two surgical approaches for displaced intra-articular calcaneal fractures: sinus tarsi versus extensile lateral approach. BMC Musculoskelet Disord 2015; 16: 63.
- Maxwell AB, Owen JR, Gilbert TM, Romash MM, Wayne JS, Adelaar RS. Biomechanical Performance of Lateral Versus Dual Locking Plates for Calcaneal Fractures. J Foot Ankle Surg 2015; 54: 830-835.
- James M, Bruce S. Minimally Invasive Screw Fixation Technique of Calcaneal Fractures. Tech Orthop 2012; 27: 94-101.
- Ibrahim T, Rowsell M, Rennie W, Brown AR, Taylor GJ, Gregg PJ. Displaced intra-articular calcaneal fractures: 15-year follow-up of a randomised controlled trial of conservative versus operative treatment. Injury 2007, 38: 848-855.