ISSN: 0970-938X (Print) | 0976-1683 (Electronic)
Biomedical Research
An International Journal of Medical Sciences
Research Article - Biomedical Research (2017) Volume 28, Issue 19
Multiple jejunal diverticula with jejunal volvulus: a case report
Yun-Jie Chen, Hai-Tao Jiang*, Guo-Sheng Gao, Hua-Dong Yan and Tian-Fei Wang
Department of General Surgery, Ningbo No. 2 Hospital, Ningbo, PR China
- *Corresponding Author:
- Hai-Tao Jiang
Department of General Surgery
Ningbo No. 2 Hospital, Ningbo
PR China
Accepted date: September 07, 2017
Jejunal diverticula are a rare clinical disease that was first reported by Sommering in 1974. Jejunal volvulus is the torsion of the jejunum and its mesentery, and is a medical emergency. There are no specific symptoms for jejunal diverticula, making this disease difficult to identify. Furthermore, this can lead to volvulus, and further lead to ileus in some cases. In this report, we present a rare case of a 54-yold male diagnosed with multiple jejunal diverticula with jejunal volvulus, aiming to further enhance the understanding of this disease.
Keywords
Jejunum, Jejunum diseases, Diverticula, Intestinal volvulus
Introduction
Jejunal diverticula are rare, and its incidence is less than 0.5% [1-3]. Since this is a multiple disease, it has also been called multiple jejunal diverticula [4]. However, its etiology remains unclear. Furthermore, most of these cases are asymptomatic, and some can cause volvulus and ileus. It is difficult to diagnose this disease, and a delay in diagnosis may seriously impact the prognosis of intestinal obstruction treatment [5,6]. In this report, we described a patient with multiple jejunal diverticula and jejunal volvulus, and further discussed its diagnosis and treatment.
Case Report
A 54-y-old male presented to our department with a one day history of upper abdominal distending pain, without anal exhaust and defecation. The patient had many such similar symptoms in the past, and these symptoms could be alleviated after treatment in a mild degree. The patient has no history of hypertension, diabetes, rheumatic disease and glucocorticoid exposure for a long time. However, the patient has a history of smoking (one pack pack/day) and drinking (half of one jin of liquor/day) for more than 30 y. Periumbilical tenderness was obvious on physical examination without other positive abdominal signs. The laboratory value was notable for neutrophils (77.9%).
Furthermore, the unenhanced Computed Tomography (CT) examination of the abdomen was performed to evaluate the patient’s condition. Results revealed swelling in parts of the small intestine, mild swirl changes of the mesenteric vessels, duodenal descending part of the diverticulum, a gallstone, a tumor in the right liver, and peritoneal effusion.
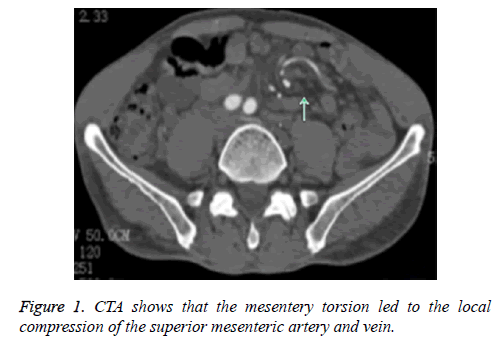
Computed Tomography Angiography (CTA) revealed that the mesentery torsion led to the local compression of the superior mesenteric artery and vein (the distal local vessel of the superior mesenteric artery was swirling at approximately one circle, and the superior mesenteric vein was obviously narrow with distal vascular expansion), hepatic hemangioma, and chronic cholecystitis with gallstone (Figure 1).
Magnetic Resonance Cholangiopancreatography (MRCP) revealed hepatic hemangioma and chronic cholecystitis with gallstone. The patient’s abdominal pain was relieved through gastrointestinal decompression and anti-infection treatment.
The patient underwent laparoscopic cholecystectomy, in which a small intestinal resection and end-to-end anastomosis was performed at day eight of hospitalization after excluding surgical contraindications.
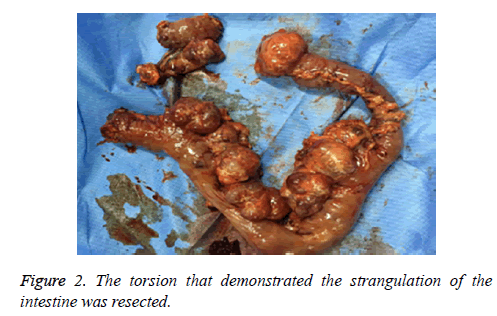
Multiple jejunal diverticula were found at the ligament of Treitz at 80 cm from the distal jejunum to 100 cm of the small intestine, and the torsion that demonstrated the strangulation of the intestine was resected (Figure 2).
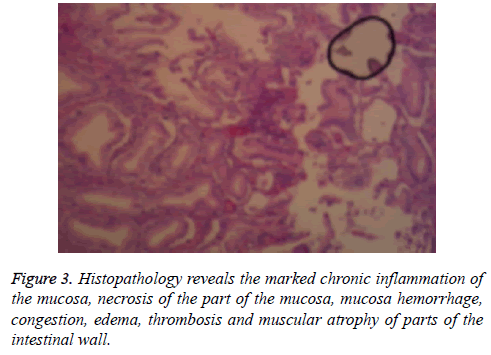
Furthermore, histopathology revealed a marked chronic inflammation of the mucosa, necrosis of the part of the mucosa, mucosa hemorrhage, congestion, edema, thrombosis and muscular atrophy of parts of intestinal wall, while there was no necrosis on both ends of the cutting edge or chronic cholecystitis with gallstone (Figure 3). The patient had an uneventful postoperative recovery, and was discharged at postoperative day six. The patient was able to eat and defecate normally in the following month, and abdominal pain did not recur. A review of the abdominal CT revealed swirling mesenteric vessels, hepatic hemangioma and a duodenal descending part of the diverticulum.
Discussion
Jejunal diverticula are rare disorders of the jejunum, which is more common in men older than 50 ys old. Jejunal diverticula are mostly false diverticula, which are mucosa and sub-mucosa that herniate through some gaps that penetrate mesenteric vessels and establish in the muscularis propria [7]. As a result, it is known to occur on the mesenteric border of the jejunum [8]. However, its specific etiology remains unclear [9]. Patients with jejunal diverticula are generally asymptomatic, and sometimes experience symptoms such as abdominal pain, abdominal distention, nausea and vomiting, melena and anemia [10]. However, jejunal diverticula has many serious complications, which include intestinal volvulus, intussusceptions, obstruction, diverticulitis, diverticulum perforation, and hemorrhage [11,12]. Furthermore, 8-30% of these complications need surgical operations [13]. What is the reason for jejunal volvulus with multiple jejunal diverticula? In the present case, we found fibrous adhesions and lumen stenosis that could be induced by jejunal diverticula inflammation between the mesentery and intestinal walls, which may interrupt intestinal location and arrangement [14]. This was the central importance. Meanwhile, many other causes have been reported, such as tumors, pregnancy, Meckel’s diverticulum, hematoma and surgical complications [15].
This disease is difficult to diagnose through clinical presentation due to nonspecific symptoms. Accessory examinations, especially for CT and angiography, could improve preoperative diagnostic accuracy [16-19]. CT scans can show “whirling signs”, the local expansion of the intestinal wall, and the thickening on the mesenteric side [20]. Angiography scans can demonstrate the twisted mesenteric vessels and dilated superior mesenteric veins. Proper preoperative management and early surgical treatment are necessary for jejunal volvulus. In order to avoid the recurrence of jejunal volvulus, jejunal fixation or appropriate resection of the jejunum should be conducted. Consequently, we first untwisted the volvulus, lysed the fibrous adhesions, removed the jejunal diverticulum, and finally rearranged the entire jejunum.
In summary, we present a case of multiple jejunal diverticula with jejunal volvulus. When a patient with multiple jejunal diverticula with jejunal volvulus is asymptomatic, CT and angiography can be helpful for its accurate and immediate diagnosis. Surgical intervention is essential for the treatment of jejunum volvulus derived from multiple jejunal diverticula.
Ethic Statement
This study complies with ethical standards.
Disclosure of Conflict of Interest
All authors have no conflict of interests to disclose.
References
- Tayeb M, Khan FM, Rauf F, Khan MM. Phytobezoar in a jejunal diverticulum as a cause of small bowel obstruction: a case report. J Med Case Rep 2011; 5: 482-486.
- Saxena D, Pandey A, Singh RA, Garg P, Roy R, Bugalia RP. Malroatation of gut with superior mesenteric artery syndrome and multiple jejunal diverticula presen. Int J Surg Case Rep 2015; 6: 1-4.
- Kassahun WT, Fangmann J, Harms J, Bartles M, Hauss J. Complicated small-bowel diverticulosis: a case report and review of the literature. World J Gastroenterol 2007; 13: 2240-2242.
- Zhang ZB, Li DY, Gu C. Diagnosis and treatment of intestinal obstruction caused by multiple jejunal diverticul. Chin J Gen Surg 2014; 29: 524-526.
- Balducci G, Dente M, Cosenza G, Mercantini P, Salvi PF. Multiple giant diverticula of the foregut causing upper gastrointestinal obstruction. World J Gastroenterol 2008; 14: 3259-3261.
- Zhang ZB, Gu C. Multiple jejunal diverticula causing intestinal obstruction. Indian J Med Res 2015; 142: 97.
- Patel VA, Jefferis H, Spiegelberg B, Iqbal Q, Prabhudesai A, Harris S. Jejunal diverticulosis is not always a silent spectator: a report of 4 cases and review of the literature. World J Gastroenterol 2008; 14: 5916-5919.
- Garnet DJ, Scalcione LR, Barkan A, Katz DS. Enterolith ileus: liberated large jejunal diverticulum enterolith causing small bowel obstruction in the setting of jejunal diverticulitis. Br J Radiol 2011; 84: 154-157.
- Singal R, Gupta S, Airun A. Giant and multiple jejunal diverticula presenting as peritonitis a significant challenging disorder. J Med Life 2012; 5: 308-310.
- Lempinen M, Salmela K, Kemppainen E. Jejunal diverticulosis:a potentially dangerous entity. Scand J Gastroenterol 2004; 39: 905-909.
- Lee BJ, Kumar P, Van den Bosch R. Jejunal diverticula: a rare cause of life-threatening gastrointestinal bleeding. J Surg Case Rep 2015; 1: 1-3.
- Balducci G, Dente M, Cosenza G, Mercantini P, Salvi PF. Multiple giant diverticula of the foregut causing upper gastrointestinal obstruction. World J Gastroenterol 2008; 14: 3259-3261.
- Falidas E, Vlachos K, Mathioulakis S, Archontovasilis F, Villias C. Multiple giant diverticula of the jejunum causing intestinal obstruction: report of a case and review of the literature. World J Emerg Surg 2011; 6: 8.
- Terada T. Diverticulitis of multiple diverticulosis of the terminal ileum. Int J Clin Exp Pathol 2013; 6: 521-523.
- Shen XF, Guan WX, Cao K, Wang H, Du JF. Small bowel volvulus with jejunal diverticulum: Primary or secondary? World J Gastroenterol 2015; 21: 10480-10484.
- Duda JB, Bhatt S, Dogra VS. Utility of CT whirl sign in guiding management of small-bowel obstruction. AJR Am J Roentgenol 2008; 191: 743-747.
- Chen PC, Redwine MD, Potts JR. Computed tomographic diagnosis of small-bowel volvulus: case report. Can Assoc Radiol J 1997; 48: 183-185.
- Kornprat P, Langner C, Mischinger HJ. Enterolithiasis in jejunal diverticulosis, a rare cause of obstruction of the small intestine: a case report. Wien Klin Wochenschr 2005; 117: 297-299.
- Feng ST, Chan T, Sun CH, Li ZP, Guo HY, Yang GQ. Multiphasic MDCT in small bowel volvulus. Eur J Radiol 2010; 76: 13-18.
- Tamura J, Kuniyoshi N, Maruwaka S, Shiroma J, Miyagi S, Orita H. “Whirl Sign” of primary small bowel volvulus. West J Emerg Med 2014; 15: 359-360.