ISSN: 0970-938X (Print) | 0976-1683 (Electronic)
Biomedical Research
An International Journal of Medical Sciences
- Biomedical Research (2016) Volume 27, Issue 2
Full-mouth periodontal examination prior to and after nonsurgical treatment in chronic periodontitis patients.
| Cátia Reis1, Maria Cristina Manzanares-Céspedes2, José Júlio Pacheco1, Filomena Salazar1, Elsa Maria Cardoso3,4* 1CESPU, Instituto de Investigação e Formação Avançada em Ciências e Tecnologias da Saúde, Rua Central de Gandra, 1317, 4585-116 Gandra PRD, Portugal 2Human Anatomy and Embryology Unit, Departament de Patologia i Terapèutica Experimental, Health University of Barcelona Campus (HUBc), University of Barcelona, 08907 L'Hospitalet de Llobregat, Barcelona, Spain 3CICS-UBI, Health Sciences Research Centre, Faculty of Health Sciences. University of Beira Interior, Av. Infante D. Henrique, 6200-506 Covilhã, Portugal 4Faculty of Health Sciences (FCS-UBI), University of Beira Interior, Av. Infante D. Henrique, 6200-506 Covilhã, Portugal |
| Corresponding Author: Elsa Maria Cardoso, Faculty of Health Sciences University of Beira Interior Portugal |
| Accepted: January 30, 2016 |
Chronic periodontitis is a pathological condition characterized by loss of the supporting tissues of the teeth. The aim of this study was to evaluate the distribution of disease sites in different areas of mouth, prior to and following short-term nonsurgical treatment, as well as the successful of treatment. Periodontal parameters, including Probing Pocket Depth (PPD), Clinical Attachment Level (CAL) and Bleeding on Probing (BOP) were recorded in each six surfaces per tooth (mesiobuccal, buccal, distobuccal, mesiolingual, lingual and distolingual), in all mouth teeth of patients with chronic periodontitis, prior to and following nonsurgical periodontal therapy. In total, 374 disease sites (PPD ≥ 4 mm) were found and constituted the sample population of this study. The prevalence of disease sites was higher at mandibular arch, in molars, and at interproximal tooth surfaces, both prior to and after treatment. There was a trend to be more prevalent on the right side of the mouth. Nonsurgical periodontal therapy resulted in a statistically significant decrease in PPD, CAL and in the percentage of BOP sites, even though with a similar pattern of disease distribution after treatment. Following treatment, molars had significantly higher PPD and CAL than other teeth. We conclude that it is important to take particular attention to specific sites in the mouth during management of patients with chronic periodontitis and that short-term nonsurgical treatment is effective in mild/moderate periodontal pockets.
Keywords |
||||||
| Chronic periodontitis, Periodontal diseases, Periodontal debridement, Periodontal pocket. | ||||||
Introduction |
||||||
| Chronic periodontitis is an inflammatory disease of the supporting tissues of teeth resulting in periodontal pocked formation and destruction of alveolar bone. This often compromises function and esthetics, and may be associated with pain and discomfort. Thus, an accurate evaluation of the oral health is important for welfare of the patients. Moreover, periodontal disease has been associated systemic diseases and conditions particularly cardiovascular diseases, low birth weight babies, diabetes, chronic kidney disease, rheumatoid arthritis and others [1,2]. Whether periodontitis as a causative role for systemic diseases or there is a common underlying mechanism, remains to be further explored [3]. Nevertheless, prevention or treatment of periodontal disease might benefit patient health and therefore should be implemented. | ||||||
| There is little doubt that an optimal examination of periodontal status of an individual consists of a whole-mouth examination. Accordingly, the gold standard procedure for evaluation of the periodontal status is full-mouth periodontal assessment that consists of inspection of six sites per tooth on all existing teeth [4]. Although in clinical practice it is time and resource consuming, in clinical research this standard method allows to investigate entire dentition and detailed site-specific information of periodontal disease. | ||||||
| Treatment for patients with chronic periodontitis aims to halt disease progression and arrest the inflammation [5]. The most widely used techniques in periodontal therapy are nonsurgical mechanic scaling and root planning. These procedures are used to remove supra- and sub-gingival bacterial deposits from surfaces of teeth [6]. The most common outcome measures used to determine the treatment success are reduction of probing pocket depths, maintaining or improvement of clinical attachment levels, and reduction of bleeding on probing [7]. Therefore, in this study we performed whole-mouth examinations prior to, and following, a short-term nonsurgical treatment, in order to test the hypothesis that the prevalence of disease sites varies among mouth location and that nonsurgical treatment is effective to treat mild/moderate periodontal pockets. | ||||||
Material and Methods |
||||||
Study population |
||||||
| In total, 374 tooth sites with probing pocket depth, PPD ≥ 4 mm (disease sites), from patients with chronic periodontitis attending the Dental Sciences Clinic at the Department of Instituto Superior de Ciências da Saúde-Norte (Gandra, Portugal; ISCS-N), were studied. Written informed consent was obtained from each patient prior to enrolment in the study and the experimental protocols were approved by the Ethics Committee of Instituto Superior de Ciências da Saúde-Norte, according to the Declaration of Helsinki. The mean ± SD age of the subjects was 48.5 ± 11.8 years, and all the subjects were Caucasian. In total, 77% were female and 23% were male. Patients were nonsmokers, with the exception of two who smoked ≤ 10 cigarettes per day and only one patient was lefthanded. Exclusion criteria included pregnancy or lactation, systemic diseases or intake of medication, such as antibiotics, anti-inflammatory agents or immunosuppressors, for six months prior to the study. None of the patients was taking anticonvulsants or hormonal therapy. None of the patients presented parafunctional or altered chewing habits, or signs of temporomandibular disorders. | ||||||
Periodontal examination |
||||||
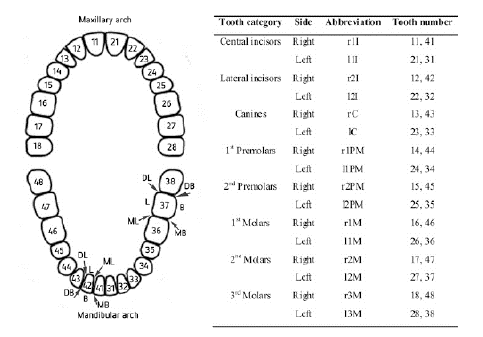
| All patients received a comprehensive periodontal examination, which included the determination of the Probing pocket depth (PPD), Bleeding on probing (BOP) and Clinical attachment level (CAL) has previously described [8]. Thus, PPD determination was performed by measuring the gingival pocket (mm) using a graduated periodontal probe (CP11; ASA Dental, Bozzano Massarosa, Italy) at each surface of the teeth in the dentition (six sites per tooth: mesiobuccal, buccal, distobuccal, mesiolingual, lingual and distolingual, Figure 1). Measurements were performed starting from the free edge of the gum to the deep groove with the probe parallel to the long axis of the tooth. BOP during the measuring of previous parameters was present or absent, and BOP positive was considered an objective sign of gingival inflammation. CAL, which represented the clinical approach of the adhesion level of the tissue to the root surface, was evaluated using the same graduated probe, corresponding to the distance (mm) between the cemento-enamel junction and the deep groove. | ||||||
Periodontal treatment and re-evaluation |
||||||
| Following periodontal examination, patients were enrolled in a nonsurgical periodontal treatment plan. Thus, after oral hygiene instructions, scaling and root planning in the affected sites, were performed using Gracey curettes (Hu-Friedy, Chicago, IL, USA) under local anesthesia. Scaling comprised the removal of tartar infragingival and root planning on the surfaces of the teeth that had a PPD of ≥ 4 mm. Following the completion of treatment, follow-up (re-evaluation) was performed. The follow-up was performed once, 2 months after treatment, in order to give the oral tissues to heal. | ||||||
Statistical analysis |
||||||
| Statistical analysis was conducted using SPSS 20.0 (IBM, Armonk, NY, USA) software and P<0.05 was considered to indicate a statistically significant difference. One-Sample Chi- Square was used to evaluate differences in the distribution of disease sites according to arches, sides (right or left), tooth categories, grouped surfaces and tooth surfaces. In each case, the null hypothesis was that the categories have equal probability. Continuous variables with a normal distribution (PPD and CAL) were expressed as the mean ± standard error of the mean, and were analyzed using parametric t-Test for paired samples (prior to and following treatment). For independent samples (different categories) we have used one way analysis of variance (ANOVA). In cases of three or more categories, Bonferroni Post Hoc Tests were used to determine the category(ies) that account for the differences within the group. McNemar's test was used to compare frequencies between related samples (percentage of disease sites within the 374 studied sites, and percentage of sites that BOP, prior to and following treatment). Pearson χ2-test was used to evaluate differences in frequency of sites that BOP within categories of each group (arch, side, tooth category, grouped surface, and tooth surface). | ||||||
Results |
||||||
Occurrence of disease sites within mouth specific locations |
||||||
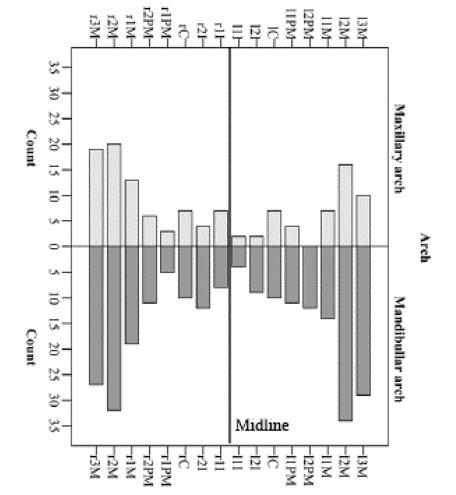
| The prevalence of disease sites varied significantly within different mouth locations. Thus, disease sites were more frequent in mandibular arch (P<0.001). Prior to treatment, 66% of the disease sites were at mandibular arch, with only 34% being in the maxillary arch (Table 1, Figure 1, and Figure 2). Following treatment there was a clinical improvement, measured by a decrease in the number of disease sites. However, a similar arches distribution was observed after treatment (Table 1). | ||||||
| Prior to treatment, there was a trend for a higher prevalence of disease sites in the right side of the mouth (P=0.098, Table 1 and Figure 2) reaching a statistically significant difference after treatment (P=0.041, Table 1). There was a significant difference among tooth categories, and molars were the most represented classes (Figure 1, Figure 2 and Table 1) both prior to and following treatment (Table 1). This was observed both at mandibular and maxillary arches (Figure 2). Interproximal portions of the teeth were the most represented diseased surfaces, while tooth mid surfaces (buccal or lingual) were the less represented (Figure 1 and Table 1). Moreover, buccal surfaces were less frequent than lingual faces (Figure 1 and Table 1). Following treatment, a similar pattern was observed (Table 1).. | ||||||
Clinical improvement after short-term nonsurgical treatment |
||||||
| Nonsurgical therapy resulted in a statistically significant decrease (P<0.001) in the PPD from an average of 4.7 mm to 3.3 mm, as well as a decrease in the CAL from 1.7 mm to 0.6 mm and in the percentage of sites with the BOP, which decreased from 55.6% prior to treatment to 38.5% following treatment (Table 2). Thus, there was a 31% reduction in bleeding on probing from baseline levels. | ||||||
Clinical parameters according to mouth locations, prior to and following treatment |
||||||
| Prior to treatment, PPD and CAL were statistically significantly lower in maxillary arch than in mandibular arch (Mean ± SEM, 4.48 ± 0.06 mm versus 4.78 ± 0.07 mm for PPD; 1.48 ± 0.06 mm versus 1.79 ± 0.07 mm for CAL, respectively, Table 3). However, following treatment there was no significant difference in PPD and CAL between arches. The percentage of sites that BOP before treatment was higher in mandibular arch (61.1%) than maxillary arch (38.9%). PPD, CAL or BOP did not differ between mouth sides (both prior to and following treatment). | ||||||
| Prior to treatment, PPD and CAL did not exhibit large variations among tooth categories, although an almost statistical difference was observed (P=0.051). Accordingly, the highest PPD means were observed in the second and third molars: 4.85 ± 0.11 and 4.80 ± 0.11, respectively (Table 3). Following treatment a significant difference was observed in PPD between lateral incisors (2.74 ± 0.22 mm) and second (3.54 ± 0.12 mm) and third molars (3.49 ± 0.10 mm). Within each tooth category, the percentage of disease surfaces that BOP varied from 4.3% (central incisors) to 29.3% (2nd molars). After treatment the percentage of disease sites that BOP was not statistically significant different among tooth category, although varied between 3.5% (2nd Premolars) to 27.8% (2nd and 3rd molars, Table 3). | ||||||
| Among grouped surfaces (mesial, mid-surfaces and distal) or tooth surfaces there was no significant difference in PPD or CAL (both prior and following treatment). Regarding the percentage of disease surfaces that BOP there was no statistical difference within grouped surfaces prior to treatment (varied from 15.9% to 42.5%). However, following treatment, a significant difference was observed among grouped faces: in mid-surfaces the percentage of BOP was 12.5%, while in mesial surfaces the percentage was 36.1% and in distal surfaces it was 51.4%. When six tooth surfaces were analyzed separately, no significant differences were observed in PPD, CAL, either prior to or following treatment. Likewise, the percentage of disease surfaces that BOP within of tooth surfaces was not significantly different. | ||||||
Discussion |
||||||
| This study we performed a full-mouth examination of periodontal parameters, including circumferential six faces clinical assessments, around all teeth, in patients with chronic periodontitis having mild to moderate disease sites, with a PPD of 4.7 mm on average. Only disease sites with PPD ≥ 4 mm were included in the study and an accurate analysis of the prevalence and extent of periodontal status both at tooth and site-specific level, prior to and following nonsurgical treatment was performed. In contrast to other studies, who included analysis in all sites present in the patients´ mouth, we aimed to evaluate disease sites only, and determine its mouth location distribution prior to and following to treatment. The present results highlight essential aspects to be considered in oral health, namely the importance to draw a special attention to tooth- and site-specific level in the clinical practice. Having used a different design approach, our data supports documented differences in disease susceptibility between teeth [9-12]. | ||||||
| First we have found a moderate symmetry of periodontal status around the midline. However there was a tendency for an increased prevalence of disease sites in the right side, which may be related with the difficulty of right-handed persons in brushing the right half of the mouth [13]. At the transversal/ horizontal plane, mandibular arch exhibited a higher prevalence of disease sites. This could also be related to great levels of biofilm due to less effective oral hygiene and proximity of the duct openings of the parotid, submandibular and sublingual glands [14]. | ||||||
| Similar to other studies the prevalence of disease sites was higher in molars, and lowest in incisors and canines [9,15-17]. Lower prevalence of incisors in maxillary than in the mandibular arch could be related to saliva from adjacent submandibular ducts, namely salivary flow and quality of saliva. Interestingly, a recent report has shown that mean bacterial counts and red and orange complex species were in higher mean counts at up and lower molar sites and at lower incisors/canines. On the other hand, the lower DNA bacterial counts found at maxillary incisors, canines and pre-molars could be due, in part, to better oral hygiene, lower levels of saliva and the action of the upper lip during chewing, speaking and smiling [14]. | ||||||
| Our data is consistent with findings of other authors, reporting that prevalence of probing depth was higher at interproximal surfaces than mid-surfaces [9,15-18]. This suggests that periodontitis might be initiated at interproximal sites. Therefore, preventive additional cleaning actions can be made to hygienic the most difficult interproximal areas. In addition, patients should be alerted and encouraged to take special attention to these aspects, namely the meaning of taking particular attention to interdental cleaning, such as using dental floss or interdental brushes. In general our study confirms a tooth-specific and site-specific disease distribution in chronic periodontitis. Some differences with other studies could be related with disease severity, population, gender and age discrepancies, since it has been shown that these factors influence the prevalence and extent of periodontal diseases [9]. Thus, extrapolation of present conclusions to other groups should be handled and regarded with care. | ||||||
| Short-term conventional scaling and root planning treatment was successful as measured by a statistically significant decrease in PPD, CAL and percentage of sites with BOP. The efficacy of this treatment is well documented [19]. Many factors influence the outcomes of nonsurgical treatment, such as de severity of pocket, furcation involvement and angular bony lesions. As already mentioned, our study focused only on mild to moderate disease sites, which may substantiate the observed efficacy of nonsurgical treatment. Thus, at least in less severe cases, a properly performed mechanical scaling and root planning can lead to good clinical outcomes. PPD, CAL and the percentage of sites affected by BOP was higher in mandibular arch and in molars prior to treatment. This reinforces the concept that these locations reveal higher severity of disease and gingival inflammation. Moreover, our study showed that periodontal pockets associated with molars responded less favorably to treatment, corroborating previous studies [20-22]. Similarly to the study of Tomasi et al. [22], our study did not include furcation involvements, reinforcing that the lower treatment result in molars may also be related to poor accessibility for sub-gingival instrumentation. In the present study we did not found differences in the efficiency of PPD reduction according to interdental or mesial/buccal surfaces as reported by D’Aiuto et al. [21]. However, as mentioned above, there are several factors affecting the outcome of treatment, which may account for these discrepancies. | ||||||
| The findings reported in this study draw attention to the importance of considering characteristics of disease site distribution in chronic periodontitis which can be essential for planning and implementation of approaches for prevention and management of the disease. Finally, regarding periodontal therapy, our case study corroborates that short-term nonsurgical treatment is effective in mild/moderate periodontal pockets. | ||||||
Acknowledgement |
||||||
| This study was supported by a grant (06-GCD-CICS-09) from Co-operativa de Ensino Superior, Politécnico e Universitário (CESPU), Portugal. The authors declare that there are no conflicts of interest in this study. | ||||||
Tables at a glance |
||||||
|
||||||
Figures at a glance |
||||||
|
||||||
References |
||||||
|